How To Use An AED
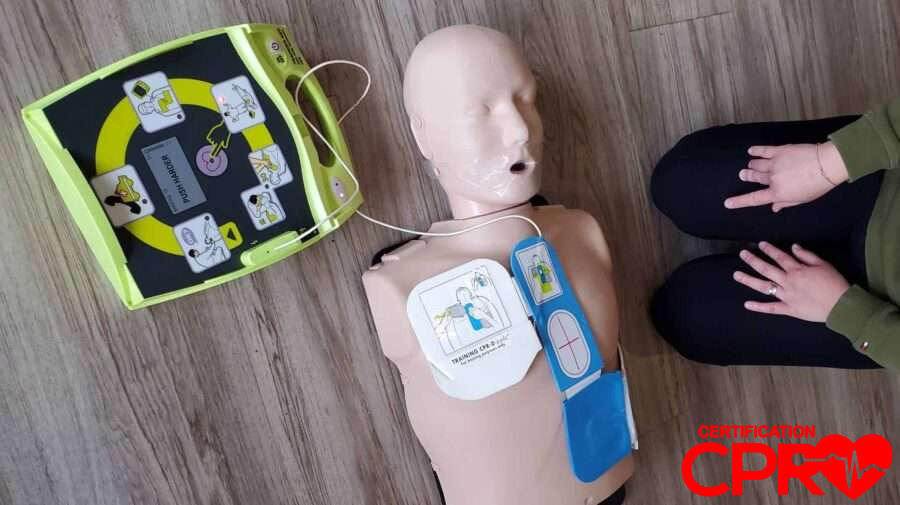
The first few seconds after someone drops, stops responding, and everybody looks at each other are where AED hesitation usually shows up. Most of the time, the device is not the hard part. The hard part is the pause before anyone commits to using it.
An AED is designed to make that moment more manageable. It gives voice prompts, checks the heart rhythm, and tells you whether a shock is advised. Your job is to get the device onto the patient quickly, follow the directions, and keep the overall response moving — which usually means going right back to CPR after analysis or a shock.
The sequence matters more than the technical language, because a person who knows the order is less likely to freeze. That matters in any building that stocks a public AED: a hotel near the airport, a convention center lobby, a large employer’s break room on the East Side — because the people already nearby become the first responders whether they planned on it or not. With El Paso EMS averaging eight to ten minutes on scene, bystanders are the bridge.
Educational note: use this information for general awareness only. It is not a substitute for calling 911, hands-on training, or professional medical judgment during an emergency.
Upcoming CPR Class Dates and Times
Know When the AED Belongs in the Response
The AED belongs in the response when the person is unresponsive and not breathing normally or is only gasping. That pattern points toward sudden cardiac arrest, not a routine fainting spell or someone who just needs a moment to recover.
If the person is awake, talking, or breathing normally, you are dealing with a different kind of emergency. But if they have collapsed and are not responding, the decision path should be immediate: call 911, start CPR, and get the AED moving toward the patient.
A lot of hesitation comes from wanting perfect certainty before acting. Cardiac arrest does not give you that kind of time. If the person is down, unresponsive, and not breathing normally, you move.
Step 1: Turn It On and Follow the Prompts
Once the AED reaches the patient, turn it on immediately. Most units begin talking the moment they power up, which is exactly what you want in a high-stress situation.
The voice prompts walk you through the sequence in order. They tell you when to attach the pads, when to stand clear, and when to resume CPR. You are not expected to invent the rescue in real time or recall every step from memory under pressure.
That built-in guidance is one reason public AEDs work as well as they do. The machine handles the analysis and the audio coaching. The rescuer handles the physical tasks: turning it on, placing the pads, clearing the patient, and getting back to compressions without delay.
Step 2: Expose the Chest and Place the Pads
AED pads go on bare skin, not over clothing. The diagrams printed directly on the pads show you where they belong, and following those pictures matters because pad placement is what allows the device to analyze correctly and — when needed — deliver a shock through the heart.
For a typical adult rescue, one pad goes on the upper right side of the chest and the other goes on the lower left side. That positioning creates the path the device expects to use. In a hands-on AHA BLS class, students practice that placement as part of the full CPR-AED sequence so it feels familiar when the moment actually arrives.
If the chest is wet — something that can happen during outdoor events in El Paso’s summer heat — dry it quickly before placing the pads. If the person has a pacemaker or another visible implant, place the pad slightly away from that area instead of directly over it. Those are normal adjustments, not reasons to stall the rescue.
Step 3: Clear the Person During Analysis and Shock
Once the pads are attached, the AED analyzes the rhythm. During that analysis, nobody should be touching the patient — the machine needs a clean read, and this is one of the moments where scene control matters most.
Look at the patient, scan the people around you, and say “clear” out loud so everyone steps back. If the device advises a shock, stay clear again while the shock is delivered. Quiet assumptions are not enough. One confident, audible “clear” command keeps the scene organized and keeps that pause short so you can return to CPR immediately.
In a crowded setting — a gym, a school cafeteria, a break room at Fort Bliss — someone often keeps a hand on the patient’s shoulder, or leans in to watch, or keeps repositioning while the device is working. Taking charge of that moment and making the clearing command visible and clear makes the whole response faster and safer.
Step 4: Resume CPR Right Away
After the AED analyzes the rhythm, it will either advise a shock or announce that no shock is advised. Either way, the response is still moving. In almost every case, the next step is to resume CPR as soon as the device tells you to.
If a shock is delivered, start compressions again when the machine instructs. If no shock is advised, start compressions again when the machine instructs. Some bystanders hear “no shock advised” and treat it like a signal that the emergency has somehow downgraded. It has not. The device simply did not detect a shockable rhythm at that moment, so compressions need to continue without pause. Non-shockable rhythms — asystole (flatline) and pulseless electrical activity (PEA), where the heart shows some electrical activity but is not pumping — cannot be corrected by a shock; the machine is not broken or withholding anything, it is accurately telling you that compressions are the right tool right now.
That back-and-forth between CPR and AED prompts is the real rhythm of the rescue. The device checks the rhythm. You do the physical work. Then the cycle repeats until EMS arrives or the person starts showing clear signs of life. Once the sequence is understood, the whole process feels far less mysterious — and far less frightening to act on.
Mistakes That Slow AED Use Down
The most common mistake is hesitation at the start. People waste critical time wondering whether they are qualified, whether they should wait for someone more experienced, or whether using the AED could somehow make things worse. The device is on the wall for exactly this situation, and you are allowed to use it. Texas’s Good Samaritan law — found at Texas Civil Practice and Remedies Code §74.151 — provides civil liability protection for ordinary citizens who act in good faith during a cardiac emergency.
Poor scene control is another common problem. Too many people crowd in, no one gives a clear command, and someone is still touching the patient during analysis. A step that should take only a moment turns messy when nobody takes charge, and those lost seconds add up.
Treating the AED as though it replaces CPR is a third way the rescue loses ground. It does not. CPR and AED use belong together in one continuous response. If compressions stop for too long or everyone stands waiting after each prompt, the rescue loses the momentum it needs.
Hands-on practice matters because the sequence has to live in your hands, not just in your head. This is the kind of emergency that starts in an office on the West Side or a classroom at EPCC, somewhere the AED is already on the wall but nobody has ever used one. The more familiar the sequence feels before that day, the faster and calmer the response will be.
