What Is CPR
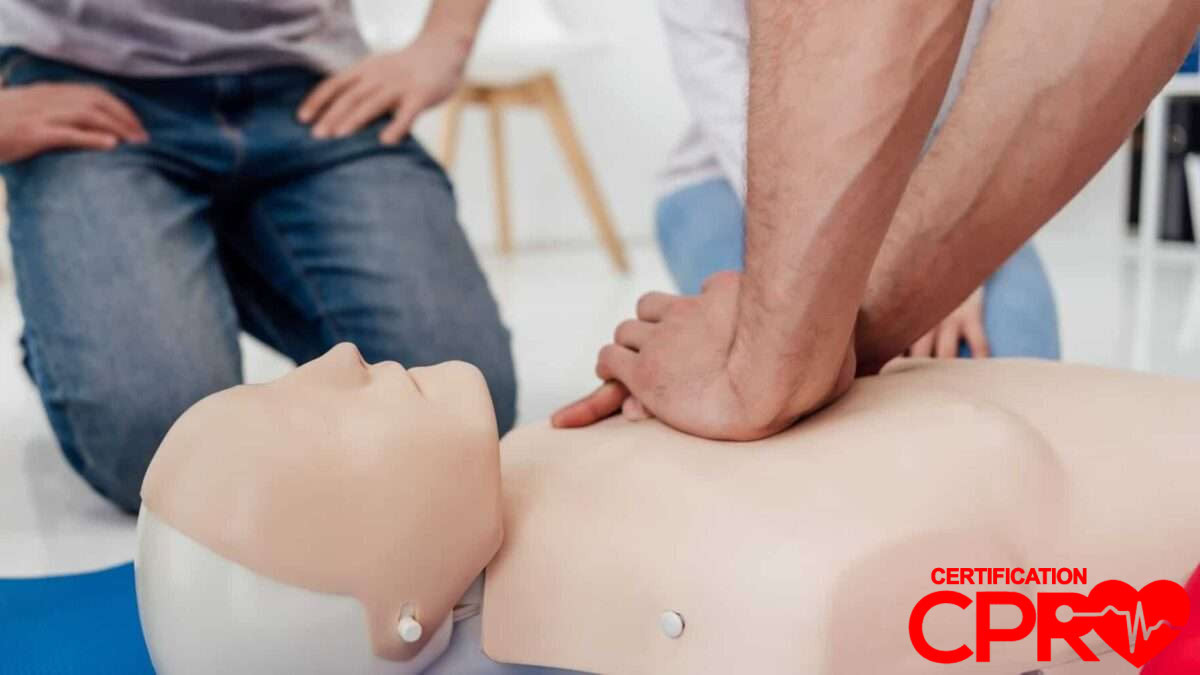
Picture a shift change at a border corridor distribution center or a lunch break at an El Paso ISD campus. Someone at a nearby table stops responding. A chair scrapes, a phone appears, and the first seconds dissolve while everyone tries to understand what they are looking at. If the person is unresponsive and not breathing normally, that interval already matters. The dispatcher has not answered yet, and El Paso Fire Department units are still eight or more minutes away. Whatever happens in that room before professionals arrive depends entirely on the people already there.
CPR gives those people a job. It does not cure cardiac arrest or fix the underlying medical problem, but it can keep blood moving through the body while the professional response is still en route. That is the practical value of CPR in a city the size of El Paso: it turns panic into a sequence of actions that can preserve the person long enough for an AED, EMS, or advanced care to take over.
The person with the first chance to help might be a coworker at Fort Bliss, a coach at a Ysleta ISD practice, a family member at a backyard gathering in the upper valley, or a stranger in line at a Northeast El Paso grocery store. Nobody schedules themselves for that role. Training matters because it decides whether the person nearest the emergency has only concern, or concern plus a practiced first move.
Educational note: this overview is not a substitute for 911, hands-on training, or professional medical judgment during an emergency.
Upcoming CPR Class Dates and Times
What Does CPR Stand For?
CPR stands for cardiopulmonary resuscitation. The name names the two body systems at the center of the emergency: the heart and the lungs.
The name sounds clinical, but the idea is plain enough. When the heart is no longer pumping blood effectively and the person is not breathing normally, CPR is the physical response for that emergency. Chest compressions press on the breastbone to help move blood through the body; rescue breaths may be added by trained rescuers; and the sequence gives the responder something concrete to follow instead of improvising under pressure.
In everyday conversation, “CPR” gets used loosely. Someone might mean chest compressions only, a class they took years ago, or a general sense of preparedness. In an emergency, the meaning narrows: CPR is the response that begins when a person is unresponsive and not breathing normally, with the goal of keeping them alive until more advanced help can take over.
What Is CPR and How Does It Work?
CPR works by creating artificial circulation when the heart can no longer perform that function on its own. As soon as effective pumping stops, blood flow to the brain and vital organs falls rapidly. Chest compressions do not restore normal circulation, but they can keep enough blood moving to slow the damage while an AED, EPFD paramedics, or advanced medical care enters the response.
For trained rescuers, adult CPR means placing the heel of one hand on the lower half of the breastbone, placing the other hand on top, locking the elbows, and pressing hard and fast at a rate of 100 to 120 compressions per minute. Adult depth is at least two inches, and the chest should return fully between compressions. Those details read simply on a page, but they are physical details. Good CPR is not light pressure; it is steady, demanding work that requires real practice to do correctly under stress.
When rescuers are trained to provide breaths, adult CPR uses a 30:2 compression-to-breath ratio. The public message is often simpler: an untrained bystander who sees a teen or adult suddenly collapse can call 911 and start continuous chest compressions without rescue breaths. Hands-Only CPR exists because hesitation is one of the main reasons bystanders do nothing, and a shorter first instruction gives more people a way to begin rather than standing in place.
CPR does not restart the heart through force. It keeps oxygenated blood moving during cardiac arrest while the larger response builds around it. When an AED is available, it becomes part of that same response because it can analyze the heart’s rhythm and deliver a shock if the rhythm is shockable. Compressions support circulation; the AED addresses the electrical problem that compressions alone cannot correct. The two tools work together rather than substituting for each other.
Every set of compressions is buying time, not finishing the emergency. The responder is keeping the situation from going completely still while the next useful resource arrives. In those first minutes, maintaining circulation is the entire job. Hands-on training matters for exactly that reason: reading about compression depth and recoil is useful, but feeling what correct compressions require on a manikin is a different experience entirely, one that holds up better when the room is loud, the patient is down, and everyone is looking for the person who will move first. For the full mechanics, the complete CPR technique guide walks through every step of the physical sequence.
When Is CPR Needed?
CPR is needed when a person is unresponsive and not breathing normally, or when they are breathing only in occasional gasps. The difficulty is not memorizing that standard; it is trusting the pattern when the scene in front of you is messy and uncertain. Delay happens because bystanders keep searching for stronger confirmation, even after the most important signs are already visible.
Agonal breathing is one of the biggest trouble spots. A person in cardiac arrest may make occasional gasping or snoring sounds that look superficially like breathing. That is not normal breathing, and treating it as such wastes critical minutes. If the person will not respond and the breathing looks wrong or irregular, the correct response is to treat it as cardiac arrest: call 911, start CPR, get the AED.
CPR is not the response for someone who is awake, talking, and breathing normally but feeling sick, dizzy, or anxious. It belongs in the collapse-and-not-breathing-normally emergency, and it needs to begin quickly. If that is what you are seeing, do not wait for more evidence. Call 911, begin compressions, and direct someone to find the nearest AED.
If you are alone with a phone, put 911 on speaker and let the dispatcher guide you while you work. That guidance helps more than most people expect. It keeps the response moving, reduces the urge to second-guess, and helps bring an AED into the scene faster if one is nearby. El Paso 911 dispatchers are trained to walk callers through compression-only CPR while units are responding.
Who Can Perform CPR?
The people most likely to perform CPR are not paramedics — they are whoever was already in the room when someone collapsed. During the first minutes of cardiac arrest, EMS is still several minutes away, and the response depends entirely on whoever is closest. In El Paso, that person is usually a coworker, a family member, a coach, a classmate, or a stranger who happened to be nearby.
Public CPR training matters because cardiac arrest does not announce itself around who is qualified to respond. It happens in ordinary settings, often in front of people who never imagined being part of the response. If nobody nearby is willing to move, the first and most important phase of the emergency is simply lost.
Not everyone responds at the same level. Someone who has practiced in an AHA BLS CPR class is better positioned to recognize the emergency, start compressions correctly, use an AED, and maintain technique through the minutes of work before EPFD arrives. But even an untrained bystander doing compressions gives the person a chance they would not otherwise have, which is exactly why Hands-Only CPR gets emphasized so heavily in public health campaigns.
Training does not turn every bystander into a clinician, but it changes what an ordinary person can do in those first minutes. Instead of looking around and waiting for someone else to move, the trained responder has a sequence: call 911, start compressions, get the AED, keep going until help takes over.
CPR Success Rates and Statistics
CPR matters because out-of-hospital cardiac arrest still carries difficult odds, and the early minutes are where bystanders can influence them. The American Heart Association’s 2026 statistics update reported 10.5% survival to hospital discharge for out-of-hospital cardiac arrest in the United States in 2024. That number is sobering, and it explains precisely why the first actions at the scene receive so much attention in public health education.
The same update reported bystander CPR in 42% of cases and public AED use in 13% of cases. Those figures point to a concrete gap between awareness and action. Many people have heard of CPR; far fewer have practiced enough to recognize the emergency clearly, start compressions without losing minutes to hesitation, and operate an AED without uncertainty. In a city as geographically spread out as El Paso, that gap has real consequences.
CPR should not be treated as a vocabulary word or a box to check on an onboarding form. It is one of the few things a bystander can actually do in the first minutes that may still change the outcome. When the heart has stopped circulating blood effectively, the time before EMS arrives is the stretch where CPR and AED use matter most. That window is short and it does not repeat.
The clearest path to genuine preparedness is to take a hands-on class and practice the full sequence until it feels familiar rather than theoretical. The AHA BLS course is where that happens: manikin practice, an AED trainer, and instructor feedback on depth, pace, and recoil. The survival statistics are also a reminder that the first person near the collapse still matters. Whether that person starts CPR, reaches for the AED, or stands back waiting shapes what the next minutes look like for the person on the ground.
